Measles Outbreaks Cost US Millions as Cases Surge Across Multiple States
Measles outbreaks are costing the United States millions of dollars in public health responses as cases surge across multiple states amid declining vaccination rates, officials warn.

Measles Outbreaks Drain Public Health Budgets as Cases Climb Across States
Measles is back. Not in a small way. Outbreaks are spreading across multiple states simultaneously, each one requiring a response that costs millions of dollars before it is contained. Public health departments are stretched. The vaccination rates that once made the US a measles-free country are no longer holding in enough communities to prevent the virus from finding purchase.
Each confirmed measles case triggers an expensive and labor-intensive public health response. Contact tracing requires identifying every person who shared an airspace with the infected individual during the contagious period — on planes, in schools, in hospitals. Measles can linger in the air of a room for up to two hours after an infected person has left. The notification radius is wide. The cost of each response, including staff time, laboratory testing, and quarantine logistics, can run into hundreds of thousands of dollars per case.
The total financial burden on US public health systems from the current outbreak cycle has not yet been officially tallied. Estimates from state health departments suggest the combined cost is already in the tens of millions of dollars and climbing.
Vaccination Rates and the Communities at Risk
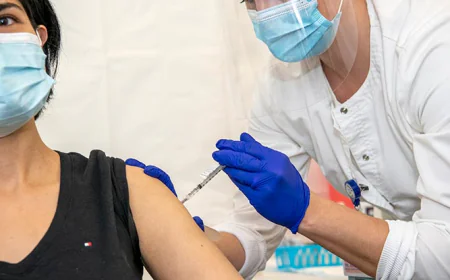
Measles vaccination rates in the United States have declined from 95% coverage — the threshold required to maintain herd immunity — in several school districts and communities across multiple states. The decline has been driven by a combination of vaccine hesitancy, the disruption to routine childhood vaccination schedules during the COVID-19 pandemic, and, in some states, loosened exemption policies that make it easier for parents to opt out of required school vaccinations.
The communities most affected by current outbreaks share a common profile: pockets of low vaccination coverage within otherwise well-vaccinated regions. Measles does not require a majority of unvaccinated people to spread — it only needs a cluster. The virus is among the most contagious pathogens known to science, with a basic reproduction number estimated at 12 to 18 in an unvaccinated population.
Hospitals near outbreak clusters are reporting increased strain on pediatric wards, particularly neonatal units where infants too young to be vaccinated are vulnerable to exposure from community spread.
Federal Response Under Political Pressure
The federal public health response has been complicated by political dynamics. Health and Human Services Secretary Robert F. Kennedy Jr. has questioned the safety of childhood vaccines, including the measles-mumps-rubella vaccine, despite overwhelming scientific consensus on its safety and efficacy. A New England Journal of Medicine editorial last month warned that leadership decisions at HHS could take generations to repair.
State health officers have been largely left to manage the outbreaks independently, without clear national coordination or messaging. CDC guidance is being issued, but implementation is uneven and in some cases actively resisted by local officials skeptical of federal health recommendations.
According to Dr. Marcus Webb, Director of Epidemiology at the Texas Department of Health Services, "Measles is a vaccine-preventable disease. Every dollar we spend responding to these outbreaks is a dollar that could have been spent on preventive care. The economic math of vaccination is not complicated."
What Containment Requires
Measles outbreak containment requires rapid case identification, exhaustive contact tracing, immediate vaccination of exposed unimmunized individuals, and consistent public communication that does not amplify vaccine hesitancy. Public health officials say several of those conditions are currently difficult to achieve simultaneously.
Vaccination clinics in affected communities are being set up on short notice. School attendance policies are being enforced more strictly in outbreak zones. But the deeper problem — the erosion of confidence in childhood vaccination that is driving the coverage decline — is not addressable through emergency response alone.
Whether the current outbreaks represent a temporary spike that will be contained by existing public health infrastructure — or the beginning of a more sustained resurgence of a disease that was declared eliminated from the United States in 2000 — will depend on decisions made in school boards, state legislatures, and federal health offices in the coming months.