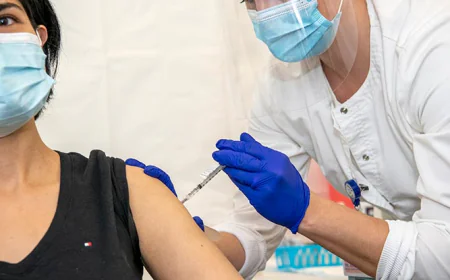
Methotrexate Shows Unexpected Heart Protection in Rheumatoid Arthritis Patients
A new study found methotrexate, one of the most widely used treatments for rheumatoid arthritis, may significantly reduce cardiovascular risk — an unexpected benefit beyond its anti-inflammatory role.
Common Arthritis Drug May Protect the Heart in Surprising New Finding
Methotrexate, one of the most widely prescribed drugs for rheumatoid arthritis and a cornerstone of autoimmune disease treatment for decades, may offer significant protection against cardiovascular disease — an unexpected secondary benefit that researchers say could reshape how clinicians think about the relationship between inflammation and heart health. The finding, published Tuesday and reported by SciTechDaily, emerged from a large observational study examining long-term cardiovascular outcomes in patients on the drug, and it adds to a growing body of evidence linking rheumatoid arthritis treatment with reduced cardiac risk.
Rheumatoid arthritis is itself an established cardiovascular risk factor. The chronic systemic inflammation associated with the disease accelerates atherosclerosis, stiffens arterial walls and elevates circulating levels of inflammatory markers linked to heart attack and stroke. Patients with poorly controlled rheumatoid arthritis have cardiovascular mortality rates significantly higher than the general population — a burden that disease-modifying drugs reduce partly by controlling inflammation, but until now not in ways that could be clearly attributed to specific agents.
The new study's finding suggests methotrexate may reduce cardiac risk through mechanisms that go beyond its control of joint inflammation — possibly including direct anti-inflammatory effects on vascular tissues, or through downstream impacts on lipid metabolism and immune cell behaviour that current models had underestimated.
Study Design and Scale
The observational study followed a large cohort of rheumatoid arthritis patients over several years, comparing cardiovascular event rates between those on methotrexate and those on other treatment regimens, while controlling for key confounding factors including age, smoking history, diabetes and pre-existing cardiovascular disease. The analysis was conducted in Australia and represented one of the largest studies of its kind in the southern hemisphere.
SciTechDaily noted Tuesday that the study found statistically significant reductions in cardiovascular event rates in the methotrexate group — a finding that held up after adjustment for confounders and across multiple subgroup analyses. The effect size was described by the study's authors as clinically meaningful, not merely statistically detectable.
Previous research into methotrexate's cardiovascular effects had produced mixed results. A large randomised controlled trial called CIRT, completed several years ago, found no cardiovascular benefit for methotrexate in a population without rheumatoid arthritis. The new study's authors argued that the CIRT population was fundamentally different — patients without the systemic inflammatory burden of rheumatoid arthritis would not be expected to show the same benefit as those with it, because the drug's cardiovascular protective mechanism appears contingent on the presence of chronic inflammatory disease.
Implications for Clinical Practice
If the findings are confirmed in prospective trials, they could influence prescribing decisions in meaningful ways. Clinicians treating rheumatoid arthritis patients with multiple cardiovascular risk factors might weigh methotrexate preference more heavily against newer biologic drugs that have different cardiovascular profiles. The findings might also prompt investigation into whether other anti-inflammatory agents used in autoimmune diseases carry similar cardiac benefits.
Separately, SciTechDaily also reported Tuesday that a new study suggested recovery from COVID-19 may not end when respiratory symptoms resolve, with evidence of persistent physiological changes in some patients lasting well beyond the acute infection phase — a reminder that the long-term sequelae of earlier pandemic waves continue to generate scientific findings years after the peak of the crisis.
According to Professor John Nanchahal, Professor of Hand, Plastic and Reconstructive Surgery at the Kennedy Institute of Rheumatology, Oxford, "The relationship between systemic inflammation and cardiovascular disease is one of the most important frontiers in medicine — and findings like this one suggest we have been underestimating how much treating the inflammation matters for the heart, not just the joints."
Whether these observational findings will translate into formal changes in clinical guidelines depends on the completion of prospective trials designed to test the cardiovascular hypothesis in controlled conditions — trials that researchers hope the new study will accelerate funding for.